At the heart of Frontier Nursing University is a talented and diverse community of students, alumni, faculty, staff, couriers and preceptors. Spotlight blogs feature members of our FNU community who are focused on the mission of educating nurse-midwives and nurse practitioners to deliver quality healthcare to underserved and rural populations.
 Since she was a child, Dr. Debra Hunt, PhD, FNP-BC, GNP-BC-CNE wanted to pursue a career in nursing. Now, she holds a PhD, has extensive experience in leadership roles on several medical boards and associations, and is an associate professor at Frontier Nursing University (FNU).
Since she was a child, Dr. Debra Hunt, PhD, FNP-BC, GNP-BC-CNE wanted to pursue a career in nursing. Now, she holds a PhD, has extensive experience in leadership roles on several medical boards and associations, and is an associate professor at Frontier Nursing University (FNU).
A resident of The Villages in Sumter County, Florida, Dr. Hunt earned her Associate Degree in Nursing from Valencia Community College in Orlando in 1991 and finished her undergraduate education at Southern Adventist University in Orlando in 1996. That same year, she enrolled in the Family Nurse Practitioner program (FNP) at the University of Central Florida (UCF) and earned her Masters in Nursing in 1998.
During this timeframe, Dr. Hunt dedicated her time to working in private practice and volunteering in her community. Through these experiences, Dr. Hunt said she became disillusioned with healthcare access in the U.S., especially in regards to those with HIV.
“I was frustrated and even angry about the way people with HIV were treated by medical professionals,” she said.
While teaching part-time at UCF in 2004, Dr. Hunt expressed her frustrations with the American healthcare system with a colleague, who challenged her to “put her money where her mouth is.” She accepted this challenge when she was accepted into UCF’s PhD program.
Through clinical practice, Dr. Hunt met several patients with young-onset dementia. Inspired by these interactions, she conducted a qualitative study to explore the lived experiences of young-onset dementia. The study took three years to complete.
“The experience changed my life,” Dr. Hunt said. “Being immersed with people my age who were living with dementia and willing to share their experience was an incredible journey.”
Dr. Hunt’s dissertation resulted in two published articles and inspired her to become an advocate for individuals with dementia. She earned her PhD in 2011.
“I was told that pursuing a PhD would change my life, and it did,” she said. “My worldview has broadened, and I see opportunities in nearly every life situation, good or bad.”
In addition to her current work with FNU, Dr. Hunt also volunteers as a primary care provider in the Central Florida area on a PRN basis.
“Caring for patients at vulnerable times in their lives is a privilege,” she said. “As a nurse practitioner, I can spend more time working with patients and the community on prevention and healthy lifestyles. NPs get to know their patients and spend the time that is needed to really impact the lives of our patients and their families.”
Over the years, Dr. Hunt has served on several medical boards and associations, and has been recognized for her work. She is the founder and was the inaugural president of the UCF Doctoral Nurses Association; was appointed by then-governor Jeb Bush to serve the South Lake Hospital Board; has served as director and as vice president of the Florida Nurses Association; received the UCF Alumni Achievement Award and participated in the development of new nurse practitioner geriatric certification through the Gerontological Advanced Practice Nurses Association. She also was heavily involved in emergency relief efforts in the aftermath of Hurricane Katrina and regularly advocates for issues central to advanced practice nursing to legislators.
Dr. Hunt said her passion for advocacy in healthcare carries over into her work with FNU.
 “In my Roles Course at FNU, I try to prepare our students to understand their roles and the importance of ‘having a seat at the table’ when it comes to healthcare advocacy and policy issues,” she said.
“In my Roles Course at FNU, I try to prepare our students to understand their roles and the importance of ‘having a seat at the table’ when it comes to healthcare advocacy and policy issues,” she said.
Dr. Hunt said she chose to work with FNU due to its reputation.
“Frontier’s reputation among other educators is very positive, even at a time when online education was suspect,” she said. “I enjoy working at Frontier because it affords me the opportunity to have more work-life balance.”
Outside of her work, Dr. Hunt enjoys spending time with her husband, three children and four grandchildren. She also enjoys volunteering, golfing, swimming, cardio drumming, watching local wildlife, fine wine and food.
Thank you, Dr. Hunt, for the extensive experience you bring as faculty member and for the excellent example you set for students at FNU.



 Frontier Nursing University (FNU), a leader in graduate nursing distance education, adjusted quickly during the pandemic to make their typical in-person clinicals
Frontier Nursing University (FNU), a leader in graduate nursing distance education, adjusted quickly during the pandemic to make their typical in-person clinicals 












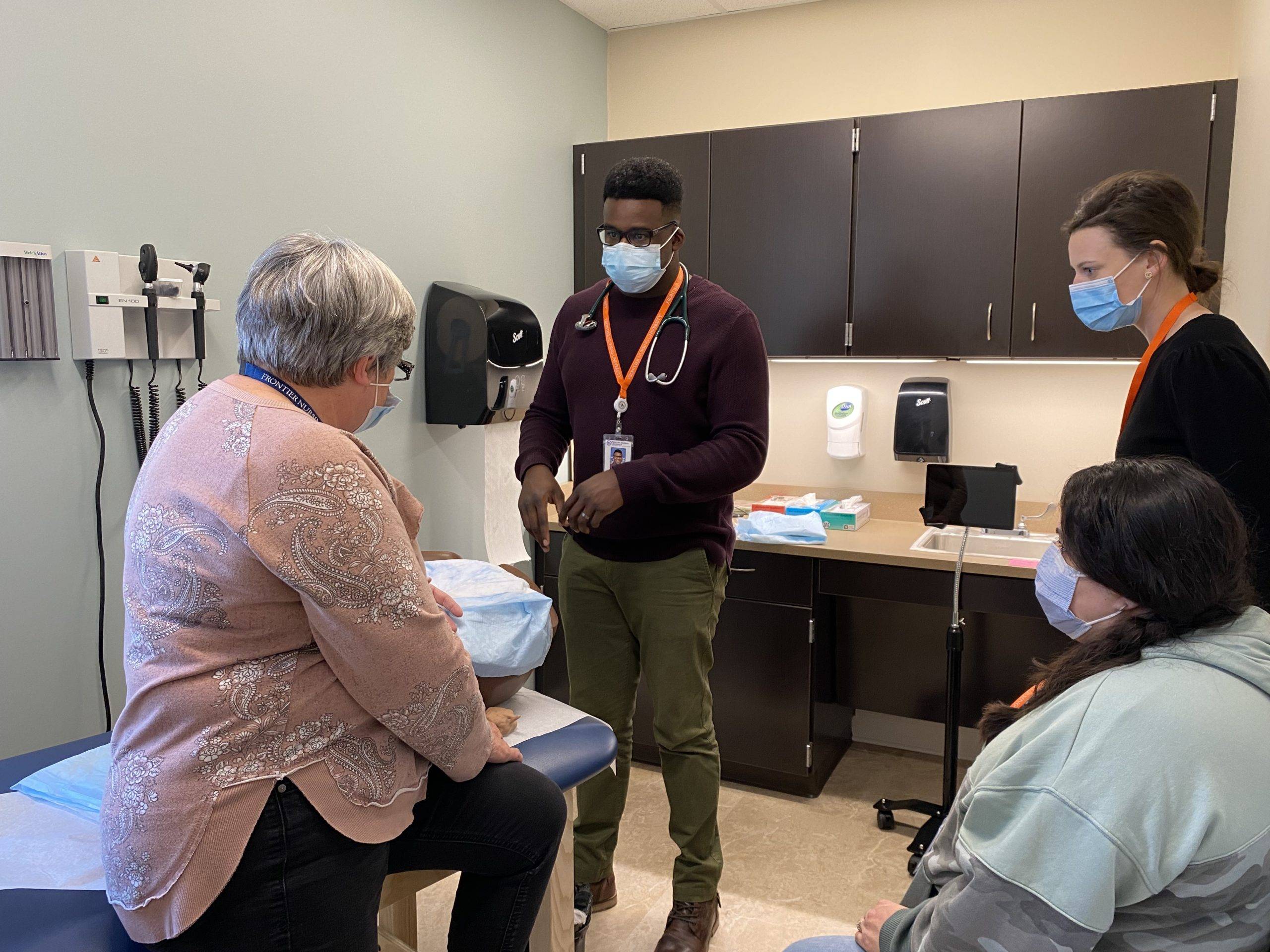











 Frontier Nursing University (FNU) student Brandon Locklear, RN, BSN, has been a traveling nurse for the past year. He works in acute hospital environments, assisting underserved communities that are facing nursing shortages. He is currently pursuing a
Frontier Nursing University (FNU) student Brandon Locklear, RN, BSN, has been a traveling nurse for the past year. He works in acute hospital environments, assisting underserved communities that are facing nursing shortages. He is currently pursuing a 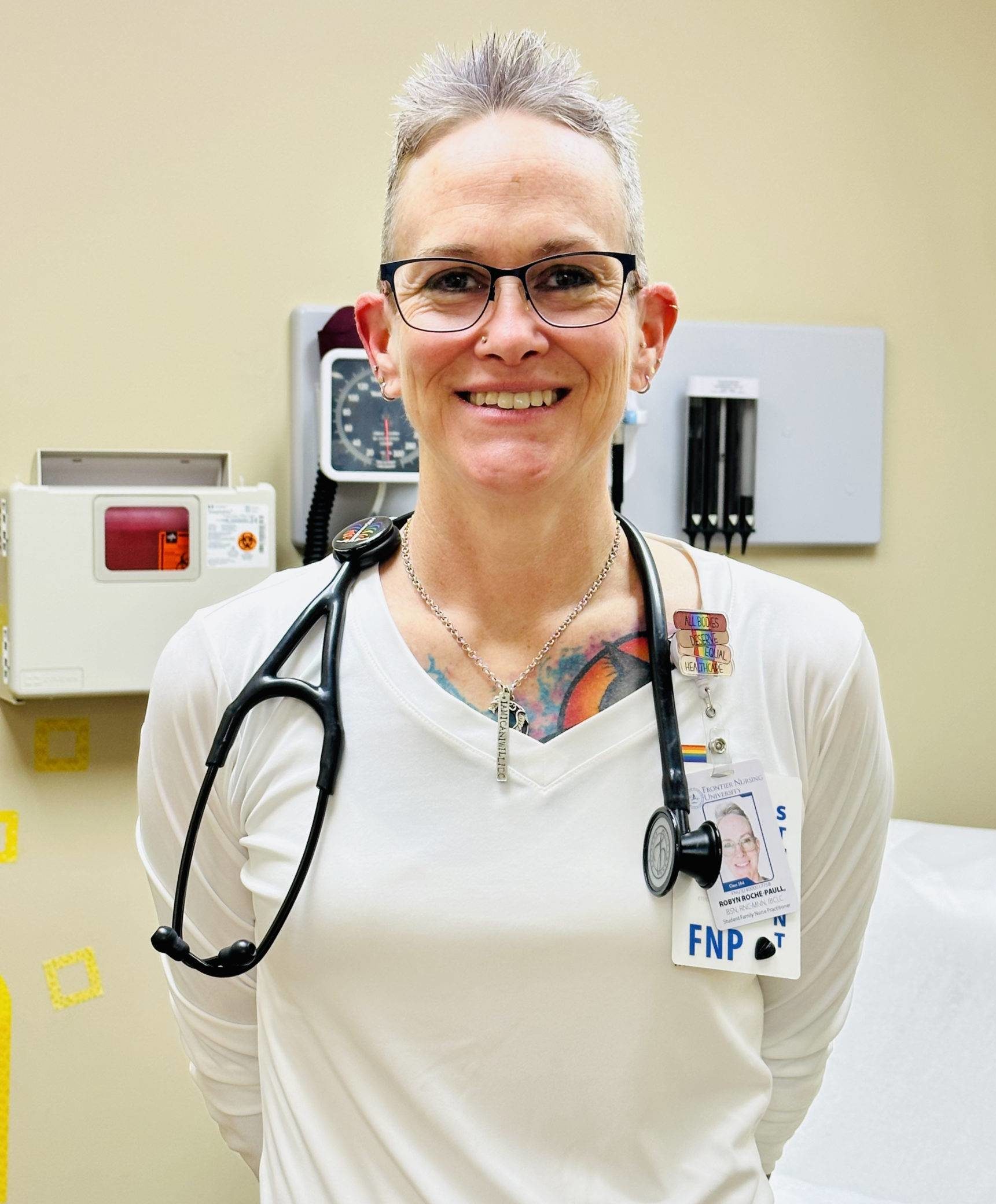
 Roche-Paull didn’t start out in the healthcare field. She was an aircraft mechanic in the U.S. Navy for six years. During this time, she met her husband and had her first child while on active duty, which brought on some major challenges. There was a lack of support and understanding for childbirth, breastfeeding, and caring for a child while on active duty. Policies weren’t in place, and it was expected that you return to your deployment six weeks after giving birth.
Roche-Paull didn’t start out in the healthcare field. She was an aircraft mechanic in the U.S. Navy for six years. During this time, she met her husband and had her first child while on active duty, which brought on some major challenges. There was a lack of support and understanding for childbirth, breastfeeding, and caring for a child while on active duty. Policies weren’t in place, and it was expected that you return to your deployment six weeks after giving birth. Soon after, Roche-Paull went back to school to receive her Bachelor of Science in Nursing (BSN) to become a registered nurse. She has since worked in labor and delivery and as a postpartum nurse. She is a two-time
Soon after, Roche-Paull went back to school to receive her Bachelor of Science in Nursing (BSN) to become a registered nurse. She has since worked in labor and delivery and as a postpartum nurse. She is a two-time  Once she graduates, Roche-Paull hopes to open a Lactation Clinic that is run by an FNP for military people. She hopes this clinic is a “one-stop shop” for pregnant people wanting to breastfeed and that she can see them during pregnancy and after. She also hopes to offer support groups through this venture.
Once she graduates, Roche-Paull hopes to open a Lactation Clinic that is run by an FNP for military people. She hopes this clinic is a “one-stop shop” for pregnant people wanting to breastfeed and that she can see them during pregnancy and after. She also hopes to offer support groups through this venture. She also asks that everyone recognize that women are veterans too.
She also asks that everyone recognize that women are veterans too.















 Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine.
Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine. Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called
Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called 










 Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College.
Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College. Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.
Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.  Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020).
Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020). Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities.
Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities. Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery.
Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery. Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan.
Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan. Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.
Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.









 Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).
Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).