 On Saturday, Sept. 26, 2020, Frontier Nursing University (FNU) hosted its first virtual commencement ceremony. The event celebrated the 817 wonderful nurse-midwives and nurse practitioners who completed the Doctor of Nursing Practice degree, Master of Science in Nursing degree, or Post-Graduate Certificate programs this year.
On Saturday, Sept. 26, 2020, Frontier Nursing University (FNU) hosted its first virtual commencement ceremony. The event celebrated the 817 wonderful nurse-midwives and nurse practitioners who completed the Doctor of Nursing Practice degree, Master of Science in Nursing degree, or Post-Graduate Certificate programs this year.
Despite the hardships this past year has brought, it is an exciting time to graduate from FNU as the University celebrates the 50th anniversary of their Family Nurse Practitioner (FNP) program and the birth of the FNP program in the United States.
It has also been a year when the world has recognized just how vital nurses and other healthcare professionals are to society, as FNU President Dr. Susan Stone shared in her address to the graduates.
“You represent the calm in the storm. You are the stabilizing force, the givers of care, and of hope,” said Dr. Stone.
This sentiment was further described by the keynote speaker for the commencement, Principal Deputy Assistant Secretary for Health, Rear Admiral (RADM) Sylvia Trent-Adams, Ph.D., RN, FAAN. RADM Trent-Adams served as the Principal Deputy Assistant Secretary for Health from January 2019 until August 2020 and has held various positions in the United States Department of Health & Human Services. A large portion of her work has been to improve access to care for poor and underserved communities, and her values align closely with the FNU mission. As expected, Trent-Adams gave a moving speech in which she inspired students to go forward into their communities and compassionately serve those who need it most.
“We as a profession stand in the crossroad of community and healthcare systems,” said Trent-Adams. “We have an obligation to deliver the best possible care with intention that includes being self-aware and conscious of our actions, our word, and our intent.”
Additional videos of faculty and staff congratulating and encouraging this year’s graduates can be found here.
Although the event took a virtual format, FNU was committed to a ceremony that retained all of the major elements of previous commencements. One of many traditions kept was honoring the students who have gone above and beyond to provide exceptional leadership to their peers. Here are the winners of this year’s Leadership Awards:
The Kitty Ernst Nurse-Midwifery Student Leadership Award: Autumn Fuselier
Women’s Health Nurse Practitioner Student Leadership Award: Gina Kristiansen
Family Nurse Practitioner Student Leadership Award: Brandy Camperlino
Psychiatric-Mental Health Nurse Practitioner Student Leadership Award: Kristin McColly
Doctor of Nursing Practice Student Leadership Award: Dr. Minyon Outlaw
Exemplary DNP Project Award: Dr. Kristin Gianelis.
A special congratulations is in order for Dr. Gianelis, who was also recently appointed as a new member of the FNU faculty!
As part of the annual commencement activities, FNU also honors the faculty members who have inspired and impacted students throughout the year. Here are this year’s student choice winners:
Student Choice Excellence in Teaching Academic Faculty Award: Dr. Eileen Thrower
Student Choice Excellence in Teaching Regional Clinical Faculty Award: Dr. Kevin Scalf.
Congratulations again to all of the spectacular students who put in the time and effort to reach these wonderful accomplishments. We are so proud to have you as part of our FNU family and cannot wait to see how you will impact nursing, nurse-midwifery, and the future of healthcare.
To watch FNU’s 2020 commencement ceremony in full, click here!



 Every October, we pause to celebrate National Midwifery Week and the important work of midwives around the globe. This year was particularly special given the World Health Organization’s (WHO) designation of 2020 as the Year of the Nurse and the Midwife.
Every October, we pause to celebrate National Midwifery Week and the important work of midwives around the globe. This year was particularly special given the World Health Organization’s (WHO) designation of 2020 as the Year of the Nurse and the Midwife.
 Family Nurse Practitioners
Family Nurse Practitioners Although FNU has expanded and introduced a range of graduate nursing degrees and specialties since 1970, they have always considered their rich foundation of reaching underserved and rural communities as they move forward. Today, Frontier is proud to have graduates providing care in all 50 states and dozens of countries. While there have been many innovations to programming throughout the years, FNU has always centered around the
Although FNU has expanded and introduced a range of graduate nursing degrees and specialties since 1970, they have always considered their rich foundation of reaching underserved and rural communities as they move forward. Today, Frontier is proud to have graduates providing care in all 50 states and dozens of countries. While there have been many innovations to programming throughout the years, FNU has always centered around the  It is a true honor to celebrate 50 years of this impactful program whose students and alumni continue to make a difference. Although Frontier has gone through many transformations since 1970, high-caliber programming continues to draw in and build leaders with a passion for reaching their communities through quality family care. With a history of compassion, trail-blazing programs and foundational support, there is little doubt that FNU will continue to pioneer healthcare, break educational barriers and celebrate many more anniversaries in its future.
It is a true honor to celebrate 50 years of this impactful program whose students and alumni continue to make a difference. Although Frontier has gone through many transformations since 1970, high-caliber programming continues to draw in and build leaders with a passion for reaching their communities through quality family care. With a history of compassion, trail-blazing programs and foundational support, there is little doubt that FNU will continue to pioneer healthcare, break educational barriers and celebrate many more anniversaries in its future.
 Twelve years ago, Frontier Nursing University (FNU) dedicated itself to providing yet another outstanding educational program,
Twelve years ago, Frontier Nursing University (FNU) dedicated itself to providing yet another outstanding educational program, 
 The Frontier community is proud to have students and alumni serving on the front lines of the COVID-19 pandemic. Throughout the next few weeks, we are committed to sharing their stories in order to provide insight, hope and encouragement. Thank you to all the health care workers who are risking their own well-being daily to serve our nation.
The Frontier community is proud to have students and alumni serving on the front lines of the COVID-19 pandemic. Throughout the next few weeks, we are committed to sharing their stories in order to provide insight, hope and encouragement. Thank you to all the health care workers who are risking their own well-being daily to serve our nation. 

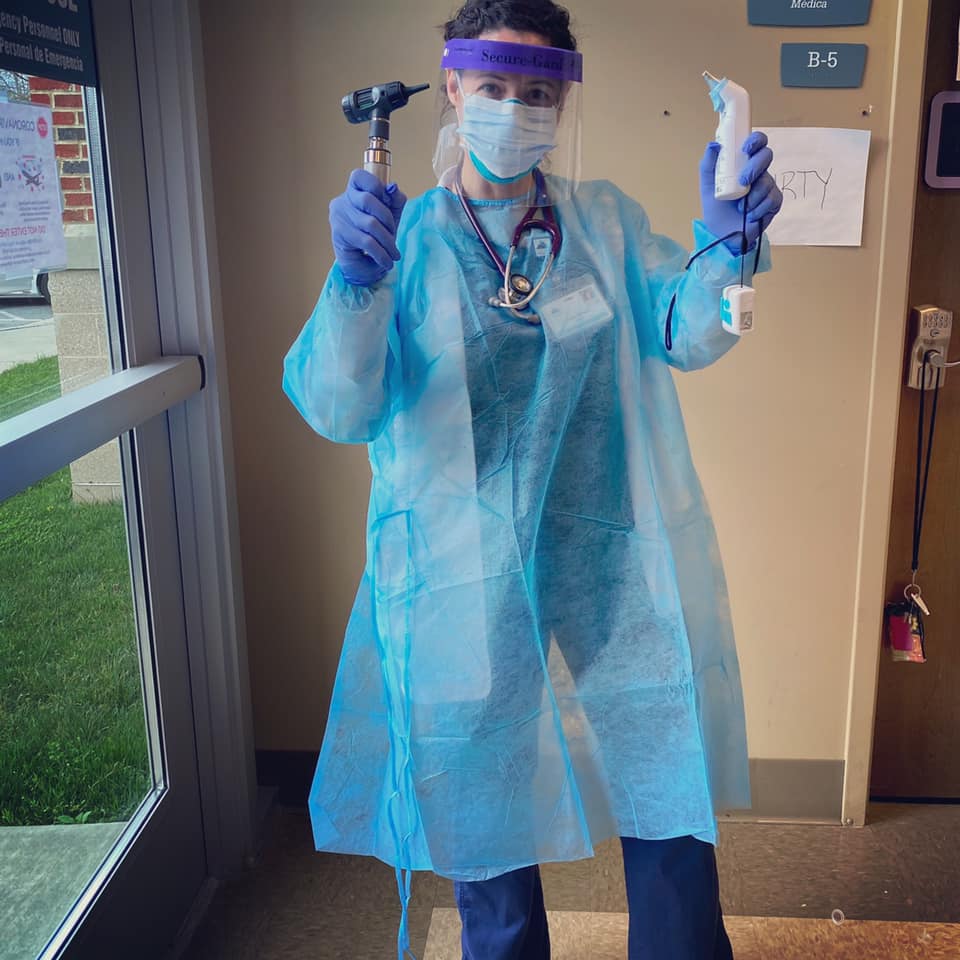
 Korah Schwab graduated from
Korah Schwab graduated from 
 In 1994, Dr. Linda Cole began her career as a nurse-midwife at the Maternity Center of East Tennessee. During Dr. Cole’s time at the maternity center, it received a new name to honor an exceptional
In 1994, Dr. Linda Cole began her career as a nurse-midwife at the Maternity Center of East Tennessee. During Dr. Cole’s time at the maternity center, it received a new name to honor an exceptional