 The National League for Nursing (NLN) recently announced that Frontier Nursing University (FNU) Associate Dean of Academic Affairs, Dr. Rachel Risner, Ph.D., DNP, APRN, C-FNP, CNE, has been selected to participate in the NLN’s Leadership Academy. The Leadership Academy, which is a year-long program, “focuses on leadership development for nurse educators and other interprofessional colleagues to develop leadership competencies, integrate social determinants of health and social change into curricula and programs, and engage in research and scholarly activities related to social determinants of health and social change.”
The National League for Nursing (NLN) recently announced that Frontier Nursing University (FNU) Associate Dean of Academic Affairs, Dr. Rachel Risner, Ph.D., DNP, APRN, C-FNP, CNE, has been selected to participate in the NLN’s Leadership Academy. The Leadership Academy, which is a year-long program, “focuses on leadership development for nurse educators and other interprofessional colleagues to develop leadership competencies, integrate social determinants of health and social change into curricula and programs, and engage in research and scholarly activities related to social determinants of health and social change.”
That is a lot to pack into one year, particularly while her plate remains full at FNU, but Dr. Risner has never been one to shy away from hard work, particularly when that work is in service to others.
Born and raised in Oklahoma, Dr. Risner is Choctaw and Cherokee. With money and resources in short supply growing up, she relied on the caring and generosity of others. Those are gifts that she has paid forward ever since.
 “If it wasn’t for the support from the Choctaw nation, I don’t know how I would have survived as a child,” Dr. Risner said. “There aren’t a lot of opportunities for tribal support in every state, but in Oklahoma, there is a lot of support from the tribes. I grew up in a very underserved family. I was lucky that I had my medical covered, that I could obtain a scholarship when I was going to school, and that I had support for clothing. I was able to obtain food when I needed food. They did so much for me growing up that I feel that’s why I do what I do. If I can help somebody else the way that I was helped, it’s really important to me.”
“If it wasn’t for the support from the Choctaw nation, I don’t know how I would have survived as a child,” Dr. Risner said. “There aren’t a lot of opportunities for tribal support in every state, but in Oklahoma, there is a lot of support from the tribes. I grew up in a very underserved family. I was lucky that I had my medical covered, that I could obtain a scholarship when I was going to school, and that I had support for clothing. I was able to obtain food when I needed food. They did so much for me growing up that I feel that’s why I do what I do. If I can help somebody else the way that I was helped, it’s really important to me.”
Dr. Risner didn’t wait long to start helping others. She began working in a psychiatric facility for geriatric patients when she was 14. Then, when she was 17, she began working as a home health aid taking care of a young boy with cerebral palsy. She cared for him for seven years and even took him into her home for three years.
“I cared for him all day long,” said Dr. Risner of the young man who sadly passed away at the age of 23. “I took him to school. I took him to prom. I walked him across the stage for graduation. We had a really close relationship. He impacted my life in so many ways. I just knew that by caring for him, I wanted to do more for people.”
She decided a good way to do that would be to become a nurse. While working full-time as a registered nurse, she graduated from Frontier in 2010 as a family nurse practitioner (FNP). She went into family practice for the next 18 months before being recruited by Oklahoma City University to help write the curriculum for their Bachelor of Science in Nursing (BSN) to Doctor of Nursing Practice (DNP) program. She went on to earn both her DNP and a Ph.D. in nursing education from Oklahoma City University. Dr. Risner began teaching at Frontier in 2014, holding various positions, including course faculty and course coordinator, before being named the Associate Dean of Academic Affairs in 2018.
“My work at Frontier focuses on having a big-picture view of the curriculum, of all programs at the university,” Dr. Risner said. “I have an eye on accreditation, making sure that we are meeting all of our competencies and essentials with all of our accrediting bodies, that we are meeting all of our expectations, and are graduating our students to be everything that our accreditors say they need to be.”
Ensuring these standards are met means identifying gaps in the curriculum. Doing so means that Dr. Risner works closely with many departments and individuals at FNU.
“We strive for consensus and collaboration in Academic Affairs to make sure we are meeting the needs of everybody in every department,” Dr. Risner said. “We can then make sure that we are producing the absolute best product that we can for our students to be successful in each one of our programs so they can meet the needs of the families that they are serving in their practice.”
 “We wanted to hear from all of our stakeholders to determine what we could do better and how we could make our curriculum more diverse, more equitable, and more inclusive for our students to assist them in being better providers in all of our programs.”
“We wanted to hear from all of our stakeholders to determine what we could do better and how we could make our curriculum more diverse, more equitable, and more inclusive for our students to assist them in being better providers in all of our programs.”
– Dr. Rachel Risner, Ph.D., DNP, APRN, C-FNP, CNE
Frontier Nursing University Associate Dean of Academic Affairs
The curriculum review process is an initiative of the President’s Diversity, Equity, and Inclusion (DEI) Task Force, which was formed in January 2021. Dr. Risner and the Curriculum and Course Design Coach Audrey Perry, DNP, CNM, began by holding meetings with students, faculty, and staff.
“We wanted to hear from all of our stakeholders to determine what we could do better and how we could make our curriculum more diverse, more equitable, and more inclusive for our students to assist them in being better providers in all of our programs,” Dr. Risner said. By the end of these sessions, she and Dr. Perry were left with hundreds of pages of information, from which they identified five themes common to the stakeholder meetings:
- Social Determinants of Health
- Health Equity
- Anti-Racism
- Cultural Safety
- Social Justice
“We are working on scaffolding these concepts across the curriculum in all of our programs, not only in our didactic courses but across our clinical courses as well, so our students can be well prepared to apply these concepts when they are in clinical practice working with families,” Dr. Risner said.
The subcommittee also worked with FNU’s Diversity and Inclusion Committee to develop guidelines for course faculty and course coordinators concerning imagery in courses.
“Being able to see it through a different lens is extremely important,” Dr. Risner said. “Having so many students from so many different backgrounds and experiences who are looking at our curriculum in different ways is just going to help us do better and make our curriculum even better.”
Dr. Risner explains that cultural understanding and awareness are extremely important in healthcare to build trust and improve communication. One of the keys to reducing healthcare disparities and improving outcomes is a better understanding of one another’s culture.
“The biggest challenge is just building trust with your patient,” Dr. Risner said. “If you go to a regular clinic, the provider comes in, and they talk really fast. They want to do it all in 15 minutes. You can’t do that with a native person. First, (a native person) won’t talk to you because they don’t trust you. It takes so much time to build rapport and trust before you can even begin the visit. That’s what’s so different about going to Indian Health Services here in Oklahoma. I may see 25 patients per day at a clinic that’s not Indian Health Services, but (there) they may only see 10 because they know they will have to go in and build trust and rapport. Just like any culture, you need to know the approach.”
That is a message that Dr. Risner is trying to communicate not only to FNU students but to nurses and healthcare providers across the country. Through her work with NLN, she is part of a workgroup that developed a toolkit for faculty to mentor American Indian and Alaskan Native students. The same group is also developing a nurse mentor portal for faculty across the United States who work with American Indian and Alaskan Native students.
“In training faculty, there is a lot of focus on unconscious bias and microaggression, on how to be a mentor, what it means to have a mentoring relationship, including the cultural aspects of what it means to work with students who have an American Indian Alaskan Native background,” said Dr. Risner.
Dr. Risner is also involved as a group coach in the NLN Step Into Leadership Program, which is aimed at Historically Black Colleges and Universities (HBCUs). Through coaching sessions, she helps senior undergraduate nursing students transition into leadership positions after graduation.
 Dr. Risner’s leadership and impact are felt in organizations large – such as FNU and NLN – and small, such as the Oklahoma Indigenous Nurses Association. Only about 18 months old, this organization was formed by a group of five Indigenous nurses, including Dr. Risner. It is the first Indigenous nurses association in the state.
Dr. Risner’s leadership and impact are felt in organizations large – such as FNU and NLN – and small, such as the Oklahoma Indigenous Nurses Association. Only about 18 months old, this organization was formed by a group of five Indigenous nurses, including Dr. Risner. It is the first Indigenous nurses association in the state.
“There were five of us that had a like-minded goal. We’re all from different tribes, and it’s really exciting. Our Facebook page has now surpassed 100 nurses that are native here in the state,” Dr. Risner said from her home in Oklahoma City.
The group meets monthly and has a guest speaker at each meeting. As the group has grown and word has spread, so has the demand to speak at a monthly meeting. Speakers are now being scheduled over a year in advance. The calendar is filling up, and, more importantly, so has the group’s influence.
“We were able to provide feedback on the American Nurses Association (ANA) racial reckoning statement,” Dr. Risner said. “They took into consideration some of our feedback – not all of it, but they did listen. They have been in contact with our tiny little group and have asked us to participate in some research with the ANA because there are not a lot of indigenous nurses associations around, so we are trying to do as much as we can.”
The group mirrors Dr. Risner, who seemingly devotes every waking minute to serving others.
“I just try to do as much as possible to help anybody I can,” she said. “I just like helping other people.”
To learn more about FNU’s DEI efforts, visit our website.


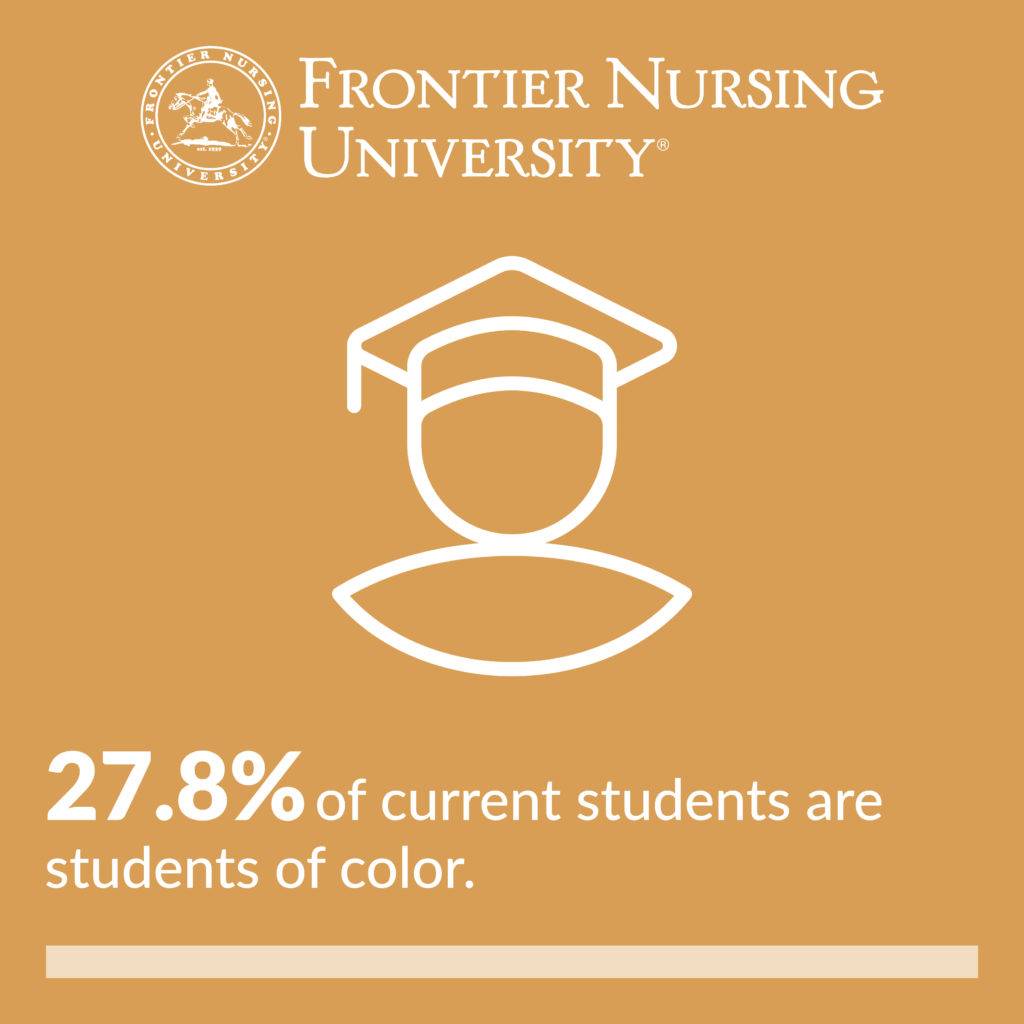 Diversity, equity, and inclusion (DEI) has been an intentional component of Frontier Nursing University’s (FNU) goals, initiatives, and planning since 2006. In 2010, the university launched PRIDE (Promoting Recruitment and Retention to Increase Diversity in Nurse-Midwifery and Nurse Practitioner Education), which has since led to the multiple DEI efforts taking place at the University today. Now known as the Diversity Impact Program, PRIDE was specifically intended to raise the level of diversity in student enrollment. In 2010, the enrollment of students of color was 9%. Today, that number has risen to over 27%, and FNU’s DEI efforts have expanded exponentially to include all members and aspects of the FNU community.
Diversity, equity, and inclusion (DEI) has been an intentional component of Frontier Nursing University’s (FNU) goals, initiatives, and planning since 2006. In 2010, the university launched PRIDE (Promoting Recruitment and Retention to Increase Diversity in Nurse-Midwifery and Nurse Practitioner Education), which has since led to the multiple DEI efforts taking place at the University today. Now known as the Diversity Impact Program, PRIDE was specifically intended to raise the level of diversity in student enrollment. In 2010, the enrollment of students of color was 9%. Today, that number has risen to over 27%, and FNU’s DEI efforts have expanded exponentially to include all members and aspects of the FNU community.
 “They will teach us how to use the qualitative data and turn it into measurable outcomes to help us make informed decisions,” Dr. Alexander-Delpech said. “It’s all about informed decisions. I don’t want to fall into project-itis, just creating one project after another without understanding the impact. I want us to know how to measure and know as an institution that we are making a difference.”
“They will teach us how to use the qualitative data and turn it into measurable outcomes to help us make informed decisions,” Dr. Alexander-Delpech said. “It’s all about informed decisions. I don’t want to fall into project-itis, just creating one project after another without understanding the impact. I want us to know how to measure and know as an institution that we are making a difference.”




 Wednesday, Oct. 5 at 6-7 p.m. ET
Wednesday, Oct. 5 at 6-7 p.m. ET
 Frontier Nursing University (FNU) alumni Stacey Eason, ARPN, CNM, PMHNP-BC, earned her
Frontier Nursing University (FNU) alumni Stacey Eason, ARPN, CNM, PMHNP-BC, earned her  “As midwives, we see people at their most vulnerable place, and lift them into one of their greatest accomplishments…Providing compassionate, non-judgmental care allows people to feel safe in seeking care for both mental health needs and substance use needs.”
“As midwives, we see people at their most vulnerable place, and lift them into one of their greatest accomplishments…Providing compassionate, non-judgmental care allows people to feel safe in seeking care for both mental health needs and substance use needs.”







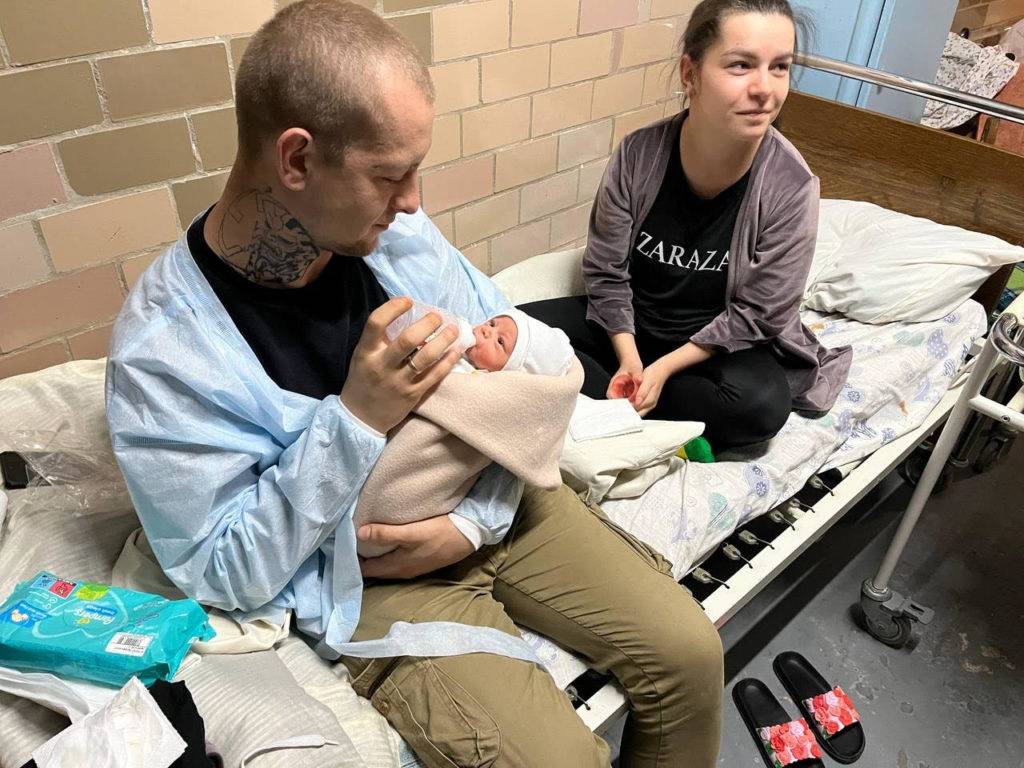
 When Russia began its attack on Ukraine in February, the images were shocking and terrifying. The heartbreaking scenes of devastation and destruction impacted everyone, but it was all particularly impactful to Frontier Nursing University (FNU) alumna Viktoriya Kashin, DNP, FNP, who was born in Russia. Her family immigrated to the United States in 1994 when she was 8. She traveled to Russia and Ukraine several times, staying connected to her homeland through friends and family. As the war began and casualties mounted, she knew she had to find a way to help. As a family nurse practitioner, Dr. Kashin, of course, is uniquely qualified to provide medical aid, and her knowledge and experience were needed in the war-torn country.
When Russia began its attack on Ukraine in February, the images were shocking and terrifying. The heartbreaking scenes of devastation and destruction impacted everyone, but it was all particularly impactful to Frontier Nursing University (FNU) alumna Viktoriya Kashin, DNP, FNP, who was born in Russia. Her family immigrated to the United States in 1994 when she was 8. She traveled to Russia and Ukraine several times, staying connected to her homeland through friends and family. As the war began and casualties mounted, she knew she had to find a way to help. As a family nurse practitioner, Dr. Kashin, of course, is uniquely qualified to provide medical aid, and her knowledge and experience were needed in the war-torn country. “The Frontier faculty and staff were extremely invested in my success and very supportive…Frontier had a lot of emphasis on rural medicine and helping underserved people. This lines up exactly with my life’s vision…Frontier helped frame my thinking and opened my eyes to many health care disparities, and is why I did not go into private practice.”
“The Frontier faculty and staff were extremely invested in my success and very supportive…Frontier had a lot of emphasis on rural medicine and helping underserved people. This lines up exactly with my life’s vision…Frontier helped frame my thinking and opened my eyes to many health care disparities, and is why I did not go into private practice.”



 Frontier Nursing University (FNU) has been named one of the best colleges in the nation to work for according to the Great Colleges to Work For® program for the second consecutive year.
Frontier Nursing University (FNU) has been named one of the best colleges in the nation to work for according to the Great Colleges to Work For® program for the second consecutive year.

 “I had never been in an environment that just brings you in, includes you, makes you feel loved and cared for. The way I think about healthcare has definitely been transformed, and this is a result of going through Frontier’s very objective DNP program. I came out of the program feeling more confident about my ability to contribute positively to any clinical quality improvement initiative.”
“I had never been in an environment that just brings you in, includes you, makes you feel loved and cared for. The way I think about healthcare has definitely been transformed, and this is a result of going through Frontier’s very objective DNP program. I came out of the program feeling more confident about my ability to contribute positively to any clinical quality improvement initiative.”















 Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine.
Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine. Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called
Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called 










 Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College.
Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College. Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.
Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.  Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020).
Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020). Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities.
Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities. Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery.
Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery. Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan.
Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan. Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.
Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.









 Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).
Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).