 When students at Frontier Nursing University prepare to begin their clinical rotations in their home communities as part of their Master of Science in Nursing (MSN) or Post-Graduate Certificate (PGC) programs, they do so with added confidence, thanks to FNU’s skills-intensive Clinical Bound.
When students at Frontier Nursing University prepare to begin their clinical rotations in their home communities as part of their Master of Science in Nursing (MSN) or Post-Graduate Certificate (PGC) programs, they do so with added confidence, thanks to FNU’s skills-intensive Clinical Bound.
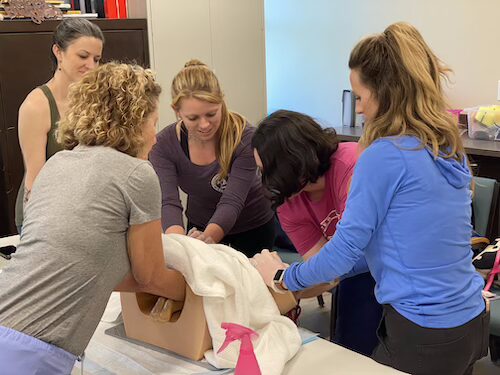
Clinical Bound, an immersive training, allows students to bridge the gap between didactic learning (online coursework) and hands-on clinical practice through simulations on FNU’s campus. The goal is to provide a safe environment where students can refine their skills, make mistakes, and correct them before working with real patients.
To effectively prepare students during Clinical Bound, FNU’s simulation labs are modeled after specific real-world environments. This provides students with practical experience in each unique setting. Our midwifery students perform simulations in an office-like setting, a home birth room, a hospital birth room, and a birthing center setting.
“Clinical Bound is an exciting time at Frontier. This is when students switch from their didactic learning to hands-on skills, so they’re with their instructors for the first time,” said FNU President Dr. Brooke A. Flinders. “It gives them a chance to validate their skills as practicing nurses, while learning through experience to trust their clinical judgment.”

In the Birth Center Room on Frontier’s campus, students gain clinical practice in an out-of-hospital setting, complete with a birthing tub and a homelike environment, where equipment is tucked away to create a comfortable atmosphere for the patient and family. Similarly, the Home Birth Room allows students to practice in a home setting, considering preemptive issues and planning for potential transfers to a hospital if complications arise.
While midwifery is often associated with home and birth centers in the U.S., The Commonwealth Fund shared 2022 data from the National Center for Health Statistics indicating that 87 percent of midwife-attended births in 2020 were in hospital settings in collaboration with nurses and physicians. Frontier’s Hospital Room provides students with the opportunity to practice using the equipment they will encounter during hospital births. The Office Visit Room is designed to simulate gynecological visits and return obstetrics appointments, and is equipped with pelvic and breast mannequins for exams, microscopes, and specimen gathering tools.
Tour our Clinical Bound simulation labs in this episode of Frontier’s On the Trail:
In the lab area, students practice a variety of skills related to gynecology and obstetrics, including maneuvers using simulators that mimic amniotic fluid and allow for different baby positions, inserting IUDs, performing endometrial biopsies, conducting cervical exams, and fetal scalp electrodes.
A unique feature of Clinical Bound is the use of standardized patients, who are trained actors portraying real-life patient scenarios. This allows students to practice both technical skills and patient communication, while faculty members, acting as preceptors, provide real-time guidance and feedback.
 Several students are able to observe these encounters in real-time thanks to a software program called SimIQ, which allows students to watch each other’s simulations from nearby classrooms or remote locations via tablets or computers. This innovative approach promotes collaborative learning allowing students to learn from each other and obtain helpful feedback from both faculty and peers.
Several students are able to observe these encounters in real-time thanks to a software program called SimIQ, which allows students to watch each other’s simulations from nearby classrooms or remote locations via tablets or computers. This innovative approach promotes collaborative learning allowing students to learn from each other and obtain helpful feedback from both faculty and peers.
By offering in-person clinical simulations and integrating SimIQ software, students are equipped with the necessary tools to interact with patients not only in a traditional in-person setting but also in a telehealth environment. This adaptability is increasingly crucial as healthcare access continues to evolve and telehealth becomes more prevalent.
By combining the knowledge gained through didactic coursework with hands-on simulation training, simulation labs during Clinical Bound equip students with the skills, confidence, and critical thinking needed for their clinical experiences. As they step into patient care roles, they do so with a solid foundation, prepared to apply their expertise in real-world settings.
To learn more about Clinical Bound on Frontier’s campus, click here.




 Advanced practice registered nurses (APRNs), which include nurse practitioners and nurse midwives, play a vital role in expanding access to healthcare, especially in underserved communities. It is important to understand the distinct role and focus of each path when considering which specialty is right for you.
Advanced practice registered nurses (APRNs), which include nurse practitioners and nurse midwives, play a vital role in expanding access to healthcare, especially in underserved communities. It is important to understand the distinct role and focus of each path when considering which specialty is right for you. For all three specialty programs, FNU students enjoy the flexibility of completing coursework online, attending full or part-time, participating in two brief on-campus immersion experiences, and fulfilling their clinical practicum in their home community. Additionally, students who earn their MSN or PGC have the option to pursue their Doctor of Nursing Practice (DNP) at Frontier afterward.
For all three specialty programs, FNU students enjoy the flexibility of completing coursework online, attending full or part-time, participating in two brief on-campus immersion experiences, and fulfilling their clinical practicum in their home community. Additionally, students who earn their MSN or PGC have the option to pursue their Doctor of Nursing Practice (DNP) at Frontier afterward.



 Frontier graduate Emily Levingston Luna, CNM, MSN, is making a significant impact on midwifery care in her home community of Las Cruces, New Mexico. As the founder of
Frontier graduate Emily Levingston Luna, CNM, MSN, is making a significant impact on midwifery care in her home community of Las Cruces, New Mexico. As the founder of  “Midwifery stood out to me as a vocation that included many of the things I feel strongly about: bodily autonomy, trauma-informed care, and reproductive justice in particular,” she said. “I chose the CNM pathway to midwifery because I wanted to be able to offer the fullest scope of care possible.”
“Midwifery stood out to me as a vocation that included many of the things I feel strongly about: bodily autonomy, trauma-informed care, and reproductive justice in particular,” she said. “I chose the CNM pathway to midwifery because I wanted to be able to offer the fullest scope of care possible.” “I think midwives tread lightly and respectfully in some of the most significant and vulnerable experiences of our clients’ lives,” Luna said of her profession. “We’re extra mindful of the weight of that, and also we’re responsible for guarding safety and providing sound, evidence-based information and guidance. We take extra time and move a little more slowly in an effort to really get to know our clients and also in an effort to help them feel known and seen.”
“I think midwives tread lightly and respectfully in some of the most significant and vulnerable experiences of our clients’ lives,” Luna said of her profession. “We’re extra mindful of the weight of that, and also we’re responsible for guarding safety and providing sound, evidence-based information and guidance. We take extra time and move a little more slowly in an effort to really get to know our clients and also in an effort to help them feel known and seen.” “I had such a supportive experience as a student at FNU, and it was helpful to hear the experiences of faculty members,” she said. “I think the variety there really helped solidify for me that practicing midwifery could look lots of ways, and empowered me to really pursue what felt right for me. I loved
“I had such a supportive experience as a student at FNU, and it was helpful to hear the experiences of faculty members,” she said. “I think the variety there really helped solidify for me that practicing midwifery could look lots of ways, and empowered me to really pursue what felt right for me. I loved 
 Frontier Nursing University recently announced that two new members have been appointed to the university’s President’s Cabinet. Jenkins Michelle Lawhorn, DNP, CNM, RNC-OB, and Chris Turley, MS, BS, will serve on the President’s Cabinet throughout 2025.
Frontier Nursing University recently announced that two new members have been appointed to the university’s President’s Cabinet. Jenkins Michelle Lawhorn, DNP, CNM, RNC-OB, and Chris Turley, MS, BS, will serve on the President’s Cabinet throughout 2025.
 The mission of Frontier’s Continuing Education Program is to create CE offerings, in collaboration with the community, that respond to the professional development needs of advanced practice nurses and midwives in the areas of scholarship, practice, entrepreneurship and service to work with all people, with an emphasis on rural and underserved communities.
The mission of Frontier’s Continuing Education Program is to create CE offerings, in collaboration with the community, that respond to the professional development needs of advanced practice nurses and midwives in the areas of scholarship, practice, entrepreneurship and service to work with all people, with an emphasis on rural and underserved communities.

















 Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine.
Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine. Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called
Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called 










 Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College.
Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College. Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.
Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.  Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020).
Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020). Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities.
Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities. Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery.
Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery. Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan.
Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan. Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.
Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.









 Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).
Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).