Every fall, Frontier Nursing University (FNU) honors alumni and individuals who go above and beyond in their service to diverse, rural and underserved populations. Please join us in congratulating the 2019 Service Award recipients.
Distinguished Service to Alma Mater, Nurse-Midwife: Stephanie Vanderhorst
The Distinguished Service to Alma Mater Award honors an alumnus who has continued to provide support to Frontier through volunteer efforts and/or donor support.
 Stephanie Vanderhorst, CNM, MSN, serves as midwifery director of Auburn Birthing Center in DeKalb, Ind. Shortly after graduating from FNU in 2002, she became the first certified nurse-midwife credentialed at DeKalb Memorial Hospital and Auburn OB/GYN; she has attended over 1,700 births since then.
Stephanie Vanderhorst, CNM, MSN, serves as midwifery director of Auburn Birthing Center in DeKalb, Ind. Shortly after graduating from FNU in 2002, she became the first certified nurse-midwife credentialed at DeKalb Memorial Hospital and Auburn OB/GYN; she has attended over 1,700 births since then.
“My goal is for every woman who wants a nurse-midwife to have a nurse-midwife by her side,” said Stephanie.
Stephanie also serves as a preceptor for CNM students. “She is a fantastic mentor and truly has a servant’s heart,” said Shannon Markle, MSN. “I have never met someone so deserving of recognition.”
In addition to practicing, Stephanie is also a leader and advocate for nurse-midwifery. She has served as the president of the Indiana American College of Nurse-Midwives and has worked with the Coalition of Advanced Practice Registered Nurses of Indiana to help bring full practice autonomy to Indiana APRNs.
Distinguished Service to Alma Mater, Nurse Practitioner: Danny Shane Webb
 Danny Shane Webb, MSN, FNP, is a nurse practitioner at Longstreet Clinic in Gainesville, Ga. He specializes in internal medicine and has hospital privileges at Northeast Georgia Medical Center.
Danny Shane Webb, MSN, FNP, is a nurse practitioner at Longstreet Clinic in Gainesville, Ga. He specializes in internal medicine and has hospital privileges at Northeast Georgia Medical Center.
Danny graduated from FNU with his Master of Science in Nursing (MSN) degree in 2017 and is currently enrolled in FNU’s Doctor of Nursing Practice (DNP) program.
As the current president of the FNU Alumni Association, he is an active, vocal, and supportive leader for the entire FNU community. Jennifer Brown, MSN, CNM, said of Danny, “He is an ever-present, enthusiastic but level-headed voice for alumni, current students and healthcare.”
Danny also serves as a preceptor for FNU students.
Distinguished Service to Society, Nurse-Midwife: Mary Kay Miller
The Distinguished Service to Society Award recognizes an alumnus who goes above and beyond to provide exceptional service in their communities.
 Mary Kay Miller, CNM, MSN, DNP, serves as Florida regional clinical faculty for FNU’s Community-based Nurse-Midwifery Education Program (CNEP) and Women’s Healthcare Nurse Practitioner (WHNP) program tracks. She has also served as a preceptor for FNU students.
Mary Kay Miller, CNM, MSN, DNP, serves as Florida regional clinical faculty for FNU’s Community-based Nurse-Midwifery Education Program (CNEP) and Women’s Healthcare Nurse Practitioner (WHNP) program tracks. She has also served as a preceptor for FNU students.
Mary Kay practiced midwifery in Fort Myers, Fla., for seven years primarily in low resource settings with underserved populations. She led the building and opening of a free-standing birth center before going on to work in Orlando for five years.
“My primary areas of clinical and academic interests are providing options to all women and supporting students,” said Mary Kay, who currently resides in Madeira Beach, Fla.
Since 2009, Mary Kay has served as the Florida Affiliate President for ACNM and has been on the board of the Florida Council of Nurse-Midwifery. She also served as the liaison for the American College of Obstetricians and Gynecologists District XII and remains active in supporting collegial relationships at the local level.
Distinguished Service to Society, Nurse Practitioner: Jessica Lynn Smith
 Jessica Lynn Smith, MSN, FNP, serves women and families as a nurse practitioner at the Vidalia Children’s Center in Vidalia, Ga. and at East Georgia Women’s Center in Statesboro, Ga. She also serves as a frequent preceptor for FNU students.
Jessica Lynn Smith, MSN, FNP, serves women and families as a nurse practitioner at the Vidalia Children’s Center in Vidalia, Ga. and at East Georgia Women’s Center in Statesboro, Ga. She also serves as a frequent preceptor for FNU students.
A two-time cancer survivor, Jessica is active in many community organizations and events. In addition to serving as the vice president of Toombs-Montgomery C.A.R.E.S, a non-profit for cancer patients, she has also organized Relay for Life teams, cancer survivor dinners, and pediatric cancer fundraisers. She frequently volunteers at a free women’s health clinic in her community.
“Although she has battled cancer twice and has been hospitalized many times, her service has never stalled,” said Jessica’s husband Brandon.
Courier Program Unbridled Spirit Award: Carlyle Carter
The Courier Program Unbridled Spirit Award is given annually to a former Courier who has carried the torch of Mary Breckinridge beyond the mountains, perpetuating the mission and spirit of Frontier in their own lives. The criteria for this award include dedication to serving others; ongoing, longstanding stewardship of Frontier; and demonstration of personal conviction, courage and a zest for adventure.
 Carlyle Carter’s first connection to FNU dates back to 1954, when she was just 11 years old. Carlyle’s grandmother was a cousin of FNU founder Mary Breckinridge, who invited Carlyle to visit her in Wendover.
Carlyle Carter’s first connection to FNU dates back to 1954, when she was just 11 years old. Carlyle’s grandmother was a cousin of FNU founder Mary Breckinridge, who invited Carlyle to visit her in Wendover.
“It was a life-changing experience,” said Carlyle, who served as a courier in 1962 and 1965. “I was excited to get to know Mary Breckinridge, the nurses, the staff, the couriers, the mountain people, and the horses. In those days, nurses were still doing home visits on horseback.”
Carlyle is currently an FNU trustee and Courier Advisory Council member. She joined the FNU Board of Directors in July 2018.
Mary Breckinridge Lifetime Service Award: Margaret Voorhies Haggin Trust
The Mary Breckinridge Lifetime Service Award recognizes an individual or organization providing longstanding support and commitment to the mission and work of Frontier Nursing Service and Frontier Nursing University.
The Margaret Voorhies Haggin Trust was created in 1938 by Margaret Voorhies Haggin in memory of her late husband, James Ben Ali Haggin.
James Haggin was born in 1827 in Frankfort, Ky. He followed the gold rush to California and acquired numerous mines, which he then sold to purchase a single tract of California land measuring 400,000 acres.
Haggin began raising thoroughbreds and bought 5,000 acres of additional land in the heart of the Bluegrass. After the death of his son, Haggin turned his attention to raising thoroughbred stock and horses at his Kentucky property, Elmendorf Farm. Haggin passed away in 1914 after building a successful business and establishing a lasting legacy.
The Margaret Voorhies Haggin Trust was created to support health and higher education. Since 1989, the Trust has provided over half a million dollars in support to Frontier Nursing University, serving a variety of needs including scholarships, renovations, and generous donations to the Versailles Capital Campaign.
We would like to thank each of these award winners for their dedication to improving the health of women and families, and their honorable representation of FNU.




 Frontier Nursing University (FNU) joined thousands of nurse-midwives across the country to celebrate
Frontier Nursing University (FNU) joined thousands of nurse-midwives across the country to celebrate 
 Frontier Nursing University (FNU) graduates, family and friends gathered to celebrate commencement on Saturday, Sep. 28. A total of 852 graduates were honored in this year’s ceremony, and 265 attended along with family, friends and over 200 FNU faculty, staff and board members.
Frontier Nursing University (FNU) graduates, family and friends gathered to celebrate commencement on Saturday, Sep. 28. A total of 852 graduates were honored in this year’s ceremony, and 265 attended along with family, friends and over 200 FNU faculty, staff and board members. FNU was honored to welcome Dr. Joycelyn Elders, M.D. as the
FNU was honored to welcome Dr. Joycelyn Elders, M.D. as the 

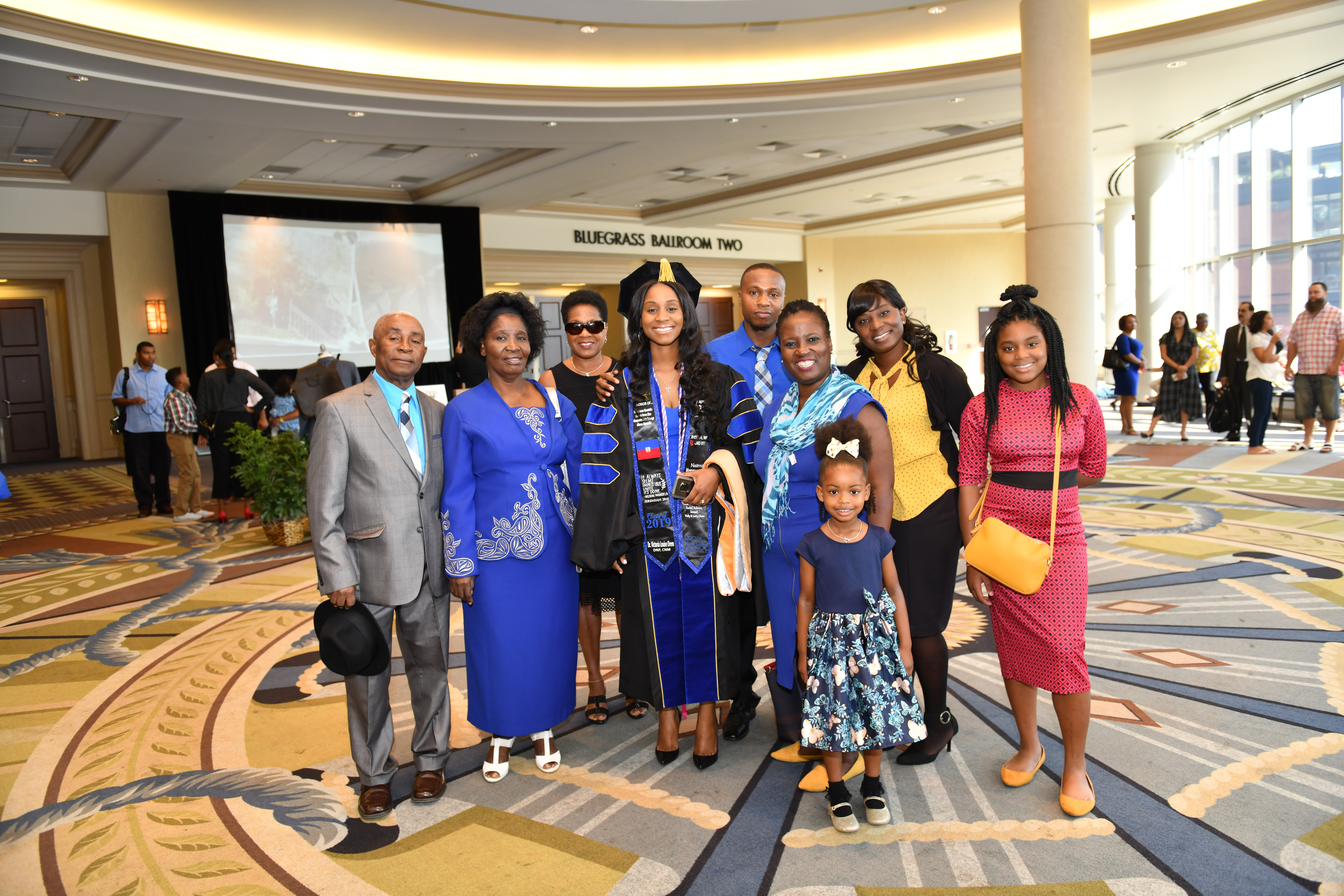




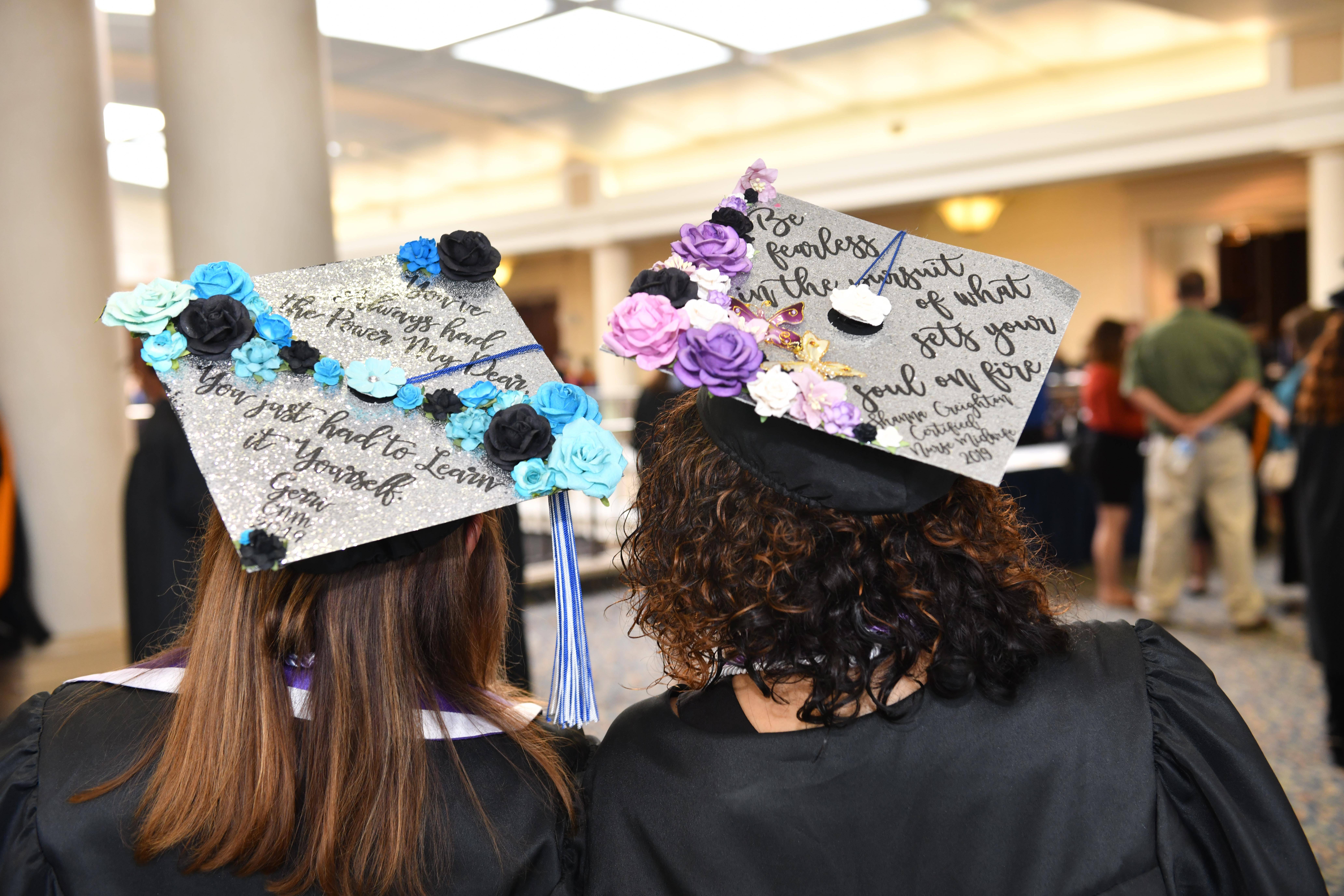

























 Frontier Nursing University (FNU) alumna and faculty member Mary Ellen Biggerstaff, MSN, DNP, has a heart for serving her community struggling with opioid addiction.
Frontier Nursing University (FNU) alumna and faculty member Mary Ellen Biggerstaff, MSN, DNP, has a heart for serving her community struggling with opioid addiction.
 Frontier Nursing University (FNU) alumna Leslie McCormack, CNM (Class 70), is passionate about serving vulnerable populations—and teaching her students to do the same.
Frontier Nursing University (FNU) alumna Leslie McCormack, CNM (Class 70), is passionate about serving vulnerable populations—and teaching her students to do the same.




 Since its foundation in 1939, Frontier Nursing University (FNU) has adopted a mission of reaching rural, diverse and underserved populations. This mission is still being lived out today, where more than 80 FNU alumni are answering the call in our country’s most remote and unforgiving state: Alaska.
Since its foundation in 1939, Frontier Nursing University (FNU) has adopted a mission of reaching rural, diverse and underserved populations. This mission is still being lived out today, where more than 80 FNU alumni are answering the call in our country’s most remote and unforgiving state: Alaska.















 Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine.
Carrie Belin is an experienced board-certified Family Nurse Practitioner and a graduate of the Johns Hopkins DNP program, Johns Hopkins Bloomberg School of Public Health, Georgetown University School of Nursing, and Johns Hopkins School of Nursing. She has also completed fellowships at Georgetown and the University of California Irvine. Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called
Angie has been a full-scope midwife since 2009. She has experience in various birth settings including home, hospital, and birth centers. She is committed to integrating the midwifery model of care in the US. She completed her master’s degree in nurse-midwifery at Frontier Nursing University (FNU) and her Doctorate at Johns Hopkins University. She currently serves as the midwifery clinical faculty at FNU. Angie is motivated by the desire to improve the quality of healthcare and has led quality improvement projects on skin-to-skin implementation, labor induction, and improving transfer of care practices between hospital and community midwives. In 2017, she created a short film on skin-to-skin called 










 Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College.
Justin C. Daily, BSN, RN, has ten years of experience in nursing. At the start of his nursing career, Justin worked as a floor nurse on the oncology floor at St. Francis. He then spent two years as the Director of Nursing in a small rural Kansas hospital before returning to St. Francis and the oncology unit. He has been in his current position as the Chemo Nurse Educator for the past four years. He earned an Associate in Nurse from Hutchinson Community College and a Bachelor of Science in Nursing from Bethel College. Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.
Brandy Jackson serves as the Director of Undergraduate Nursing Programs and Assistant Educator at Wichita State University and Co-Director of Access in Nursing. Brandy is a seasoned educator with over 15 years of experience. Before entering academia, Brandy served in Hospital-based leadership and Critical Care Staff nurse roles. Brandy is passionate about equity in nursing education with a focus on individuals with disabilities. Her current research interests include accommodations of nursing students with disabilities in clinical learning environments and breaking down barriers for historically unrepresented individuals to enter the nursing profession. Brandy is also actively engaged in Interprofessional Education development, creating IPE opportunities for faculty and students at Wichita State. Brandy is an active member of Wichita Women for Good and Soroptimist, with the goal to empower women and girls. Brandy is a TeamSTEPPS master trainer. She received the DASIY Award for Extraordinary Nursing Faculty in 2019 at Wichita State University.  Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020).
Dr. Sabrina Ali Jamal-Eddine is an Arab-disabled queer woman of color with a PhD in Nursing and an interdisciplinary certificate in Disability Ethics from the University of Illinois Chicago (UIC). Dr. Jamal-Eddine’s doctoral research explored spoken word poetry as a form of critical narrative pedagogy to educate nursing students about disability, ableism, and disability justice. Dr. Jamal-Eddine now serves as a Postdoctoral Research Associate in UIC’s Department of Disability and Human Development and serves on the Board of Directors of the National Organization of Nurses with Disabilities (NOND). During her doctoral program, Sabrina served as a Summer Fellow at a residential National Endowment of the Humanities (NEH) Summer Institute at Arizona State University (2023), a summer fellow at Andrew W. Mellon’s National Humanities Without Walls program at University of Michigan (2022), a Summer Research Fellow at UC Berkeley’s Othering & Belonging Institute (2021), and an Illinois Leadership Education in Neurodevelopmental and related Disabilities (LEND) trainee (2019-2020). Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities.
Vanessa Cameron works for Vanderbilt University Medical Center in Nursing Education & Professional Development. She is also attending George Washington University and progressing towards a PhD in Nursing with an emphasis on ableism in nursing. After becoming disabled in April 2021, Vanessa’s worldview and perspective changed, and a recognition of the ableism present within healthcare and within the culture of nursing was apparent. She has been working since that time to provide educational foundations for nurses about disability and ableism, provide support for fellow disabled nursing colleagues, and advocate for the disabled community within healthcare settings to reduce disparities. Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery.
Dr. Lucinda Canty is a certified nurse-midwife, Associate Professor of Nursing, and Director of the Seedworks Health Equity in Nursing Program at the University of Massachusetts Amherst. She earned a bachelor’s degree in nursing from Columbia University, a master’s degree from Yale University, specializing in nurse-midwifery, and a PhD from the University of Connecticut. Dr. Canty has provided reproductive health care for over 29 years. Her research interests include the prevention of maternal mortality and severe maternal morbidity, reducing racial and ethnic health disparities in reproductive health, promoting diversity in nursing, and eliminating racism in nursing and midwifery. Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan.
Dr. Lisa Meeks is a distinguished scholar and leader whose unwavering commitment to inclusivity and excellence has significantly influenced the landscape of health professions education and accessibility. She is the founder and executive director of the DocsWithDisabilities Initiative and holds appointments as an Associate Professor in the Departments of Learning Health Sciences and Family Medicine at the University of Michigan. Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.
Dr. Nikia Grayson, DNP, MSN, MPH, MA, CNM, FNP-C, FACNM (she/her) is a trailblazing force in reproductive justice, blending her expertise as a public health activist, anthropologist, and family nurse-midwife to champion the rights and health of underserved communities. Graduating with distinction from Howard University, Nikia holds a bachelor’s degree in communications and a master’s degree in public health. Her academic journey also led her to the University of Memphis, where she earned a master’s in medical anthropology, and the University of Tennessee, where she achieved both a master’s in nursing and a doctorate in nursing practice. Complementing her extensive education, she completed a post-master’s certificate in midwifery at Frontier Nursing University.









 Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).
Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).