The Frontier community is proud to have students and alumni serving on the front lines of the COVID-19 pandemic. We are committed to sharing their stories in order to provide insight, hope, and encouragement. Thank you to all the health care workers who are risking their own well-being daily to serve our nation. Click here to read more stories of courage and dedication.
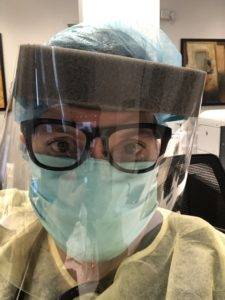 Everyone understands that working on the front lines of the COVID-19 Pandemic comes with inherent risk. Working as a nurse practitioner at Metro Immediate and Primary Care, which is part of the George Washington University Medical Faculty Associates, in Washington, D.C., Michelle Cochran, MSN, FNP, Class 71, experienced that risk first hand. When the pandemic hit, her clinic began providing assessment and testing for COVID-19 to help ease some of the demand on the hospital. Then, in April, she tested positive for the coronavirus.
Everyone understands that working on the front lines of the COVID-19 Pandemic comes with inherent risk. Working as a nurse practitioner at Metro Immediate and Primary Care, which is part of the George Washington University Medical Faculty Associates, in Washington, D.C., Michelle Cochran, MSN, FNP, Class 71, experienced that risk first hand. When the pandemic hit, her clinic began providing assessment and testing for COVID-19 to help ease some of the demand on the hospital. Then, in April, she tested positive for the coronavirus.
“I started out thinking maybe I just had a cold,” Michelle said. “Initially I was sneezing and had nasal congestion, but by the evening I had a headache and felt a bit achy. That was five days after a known exposure, so I was tested the following day. My main symptoms were headaches and low-grade fever but I did develop secondary pneumonia at the end of week two. I would say it took three to four weeks to recover. I was retested negative at three-and-a-half weeks and returned to work after four weeks.”
While some might be understandably hesitant after such an experience, Michelle felt obligated to do more upon her return to work. She continues to take the proper precautions to prevent another infection, but she also intends to donate convalescent plasma and argues that she should be even more involved on the front lines.
“I feel I should take more of the testing shifts and potential exposure since I have the gift of antibodies,” she said.
Michelle has passed on the commitment to help others to her college-age son, who tested positive for COVID-19 in March. After recovering, he donated convalescent plasma at Johns Hopkins as part of a National Institutes of Health study and encouraged her to do the same after she recovered.
Michelle admits that the pandemic has brought more than a few moments of worry and doubt, but said she leaned on her experience at FNU as a reminder of her calling.
“When my clinic started to do COVID-19 testing in early March, I had a couple of days where I thought, ‘This isn’t what I signed up for as a primary care FNP,’” Michelle said. “But then I realized this is not what anyone signed up for, but it is what is needed in my community now. In that way, it is exactly what I signed up for as a community-based family nurse practitioner from FNU.”
When she’s not dealing with COVID-19, Michelle is part of a primary care practice that also features an adjacent urgent care clinic, where she also sees patients. Michelle moved to Washington, D.C., when she was four and it is where she continues to work, live, and raise her family. She says the racial disparity for COVID cases has been eye-opening.
“The racial disparity here in COVID severity is huge,” she said. “The percentage of patients testing positive for COVID who are Black is 46 percent, but the percentage of COVID deaths who are Black is 75 percent. The city has done an admirable job with testing availability and opening testing sites in wards of the city that do not have proximity to health care. But the fact that African American/Black people are dying from COVID complications in high numbers shows a disparity that we need to address at the root. Yes, the levels of hypertension, diabetes, hyperlipidemia are high in this group in D.C., but why?”
“I believe we are seeing the physical effects of the stress of being Black in this country,” Michelle said. “It is not something that will be easy to address, but now is the time. It’s past time. It is a public health issue.”
From one healthcare crisis to the next, expect Michelle to be on the front lines, serving her community.















 Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).
Dr. Tia Brown McNair is the Vice President in the Office of Diversity, Equity, and Student Success and Executive Director for the Truth, Racial Healing, and Transformation (TRHT) Campus Centers at the American Association of Colleges and Universities (AAC&U) in Washington, DC. She oversees both funded projects and AAC&U’s continuing programs on equity, inclusive excellence, high-impact practices, and student success. McNair directs AAC&U’s Summer Institutes on High-Impact Practices and Student Success, and TRHT Campus Centers and serves as the project director for several AAC&U initiatives, including the development of a TRHT-focused campus climate toolkit. She is the lead author of From Equity Talk to Equity Walk: Expanding Practitioner Knowledge for Racial Justice in Higher Education (January 2020) and Becoming a Student-Ready College: A New Culture of Leadership for Student Success (July 2016 and August 2022 Second edition).